Recurring Bunions: Causes, Symptoms, and Treatment Options
Last updated: 2026-02-23T04:13:44.646Z
Author: Dr. Sarah Patel, DPM
Key takeaways (TL;DR)
- A recurring bunion often needs a mix of footwear changes, protective products, exercises, and sometimes surgery if cartilage loss is advanced. [1][2]
- Use wide-toe-box shoes, bunion sleeves or tailor’s sleeves, orthotics, and toe mobility exercises to reduce pain and slow progression. [3][4]
- If you have worsening stiffness, daily activity limits, or X-ray evidence of cartilage loss, talk with a podiatrist about imaging and surgical options. [2][5]
Direct answer
Recurring bunions most often improve with targeted conservative care: wide shoes, protective sleeves or padding, orthotics, and daily toe exercises. If cartilage loss limits motion or pain is severe, surgical options focused on joint preservation or fusion may be needed.
4.9 ⭐⭐⭐⭐⭐ ( 1843 reviews )
What is a bunion (hallux valgus) and bunionette (tailor’s bunion)
- Bunion (hallux valgus): a bump at the base of the big toe. The big toe leans toward the second toe. Bones shift and soft tissue change. Pain and shoe rubbing are common. [1][2]
- Bunionette (tailor’s bunion): a similar bump on the outer edge of the foot at the little toe. It causes lateral pressure and rubbing. The same shoe rules apply. [1]
Symptoms and when to seek care
Common signs a bunion is returning
- New or increasing bump at the big-toe joint.
- Stiffness or loss of range of motion in the big toe.
- Pain when walking, standing, or wearing shoes.
- Redness, callus, or skin breakdown where the shoe rubs.
- X-ray evidence of joint space narrowing (cartilage loss) or bone spurs. [2][5]
When to see a podiatrist
- You can’t fit normal shoes.
- Pain limits daily tasks or exercise.
- Stiffness or loss of toe motion develops.
- X-rays show cartilage thinning or arthritis. [2][5]
Why recurring bunions happen
- Genetics: some foot shapes are prone to hallux valgus. [2]
- Incomplete correction: surgery may not fully restore joint mechanics. [2][3]
- Cartilage loss (big toe arthritis / hallux rigidus): increases stiffness and pain. [5]
- Poor footwear and activity habits: narrow shoes and high heels add pressure. [1][6]
- Post-op factors: swelling, scar tissue, and weak rehab steps can lead to recurrence. [3]
Conservative management options and product use guidance
What works for many people
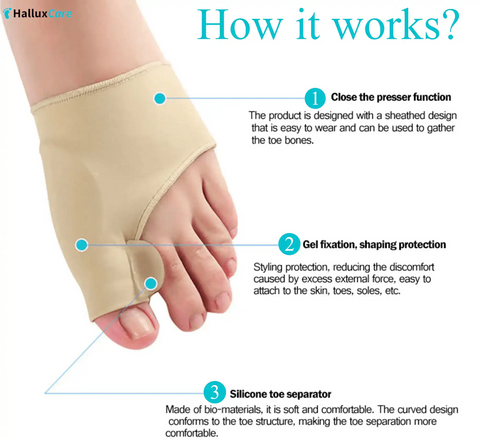
- Bunion sleeves and pads: reduce friction and redistribute pressure. Use soft sleeves for comfort and silicone splints for gentle realignment. (See the Orthopedic Bunion Pain Relief & Correction Sleeve.) [3]
- Tailor’s sleeves for bunionette protection: place on outer edge to prevent shoe rubbing. (See the Tailor’s Bunion Bunionette sleeves.)
- Arch support or orthotics: correct standing mechanics and take stress off the first metatarsal. Consider custom orthotics if simple measures fail. [3][4]
- Padding and metatarsal pads: relieve forefoot pressure and metatarsalgia.
- Topical soothing oils or creams: for skin comfort and hydration (for example, the Jamaica Black Castor Oil Soothing Oil link). Use on intact skin to reduce dryness and cracking.
Evidence highlights
- Non-surgical treatments reduce symptoms but do not always stop structural progression. [3][4]
- Surgery may be needed when cartilage loss, pain, or function are not helped by conservative care. [2][3]
Fit and footwear tips (wide toe box, materials, heel height)
- Choose a shoe with a roomy toe box. Your toes should splay naturally.
- Favor soft, stretchable uppers (mesh, soft leather) to avoid rubbing.
- Avoid narrow, pointy toe shapes and high heels above 2 inches.
- Check width with socks you usually wear. Try shoes at the end of the day when feet are swollen.
- Use removable liners or insoles to test different orthotic options. [6]
Exercises and daily routines to keep the joint mobile
- Toe range-of-motion: gently bend and straighten the big toe 10 times, three times a day.
- Towel scrunches: place a towel on the floor and pull it toward you with your toes, 2 sets of 10.
- Marble pickup: pick up marbles with toes to strengthen intrinsic foot muscles.
- Stretch calf muscles daily: tight calves change foot mechanics and add forefoot stress.
- Short walks in supportive shoes to keep mobility and control pain.
How to use bunion sleeves, splints, and spacers — simple routine
- Morning: put on a bunion sleeve before shoes if you plan activity. Use a sock over the sleeve for extra hold.
- During the day: wear orthotics or supportive shoes. Use pads or metatarsal cushions if the ball of the foot hurts.
- Evening: do toe range-of-motion exercises and gentle self-massage. Use silicone spacers at night if recommended by your provider.
- Clean sleeves per product care instructions. Replace when stretched or torn.
Practical tips and real-world applications
- Shoe shopping habit: buy shoes mid-to-late afternoon and bring your usual socks.
- Office workers: wear roomy shoes to work and carry a dress shoe option with a softer toe box.
- Runners and sports: choose wide, well-cushioned running shoes and swap them every 300–500 miles.
- Post-surgery: follow rehab steps and use recommended orthotics to lower recurrence risk. [3]
- Regional note: access to specialized foot surgeons varies by state. If local care is limited, ask about telehealth follow-up options.
Mini checklist to bring to your podiatry visit
- Recent X-rays or imaging if available.
- Notes on shoe types and daily activities.
- Timeline of symptoms and any prior surgery.
- Which conservative devices (sleeves, orthotics) you tried and how long.
Glossary of key terms and synonyms
- Bunion (hallux valgus): bump at the base of the big toe. Also called hallux valgus.
- Bunionette (tailor’s bunion): bump at the outside edge of the little toe. Also called tailor’s bunion.
- Toe spacers: small separators that sit between toes to reduce crowding.
- Sleeves: soft fabric or silicone covers that cushion the bunion and reduce friction.
- Orthoses (orthotics): shoe inserts that change foot mechanics and load distribution.
FAQs
Are toe spacers safe for bunions?
Toe spacers are generally safe for short-term use. They help reduce toe crowding and relieve rubbing inside shoes. Use soft silicone spacers and start with 15–30 minutes a day, building time as comfortable. If spacers cause new pain or numbness, stop and reassess with a clinician. [3][6]
How long should I wear toe spacers daily?
Start with 15–30 minutes at a time and increase gradually to several hours as tolerated. Many people wear them during low-activity periods, like sitting or sleeping, but not during intense exercise unless advised by a clinician. Comfort and circulation are key. [3]
Bunion vs tailor’s bunion — what’s the difference?
A bunion involves the big toe joint (medial side). A tailor’s bunion, or bunionette, is on the little-toe side (lateral edge). Both involve bony bumps and friction from shoes. Treatments and shoe advice overlap, but the specific location changes padding and corrective devices used. [1]
Do bunion sleeves help with shoe comfort?
Yes. Sleeves cushion the bump and reduce rubbing. They also shift pressure away from the skin. Sleeves help with comfort but may not correct bone alignment. Combine sleeves with wider shoes and orthotics for best results. (See the Orthopedic Bunion Pain Relief & Correction Sleeve.) [3]
When should I see a podiatrist?
See a podiatrist when pain limits your activities, when toe motion is stiff or reduced, or if X-rays show cartilage loss or bone spurs. A podiatrist will review non-surgical steps and discuss imaging and surgical options if needed. [2][5]
Can I run or play pickleball with a bunion?
You can often continue low- to moderate-impact sports with proper footwear, padding, and orthotics. Choose shoes with a wide toe box and good cushioning. If pain increases during or after play, reduce intensity and review your gear and mechanics with a specialist. [6]
Additional questions
What does cartilage loss mean for my bunion?
Cartilage loss indicates early arthritis (hallux rigidus) at the first MTP joint. It causes stiffness, pain with push-off, and may reduce effectiveness of conservative options. Discuss joint-focused procedures if function declines. [5]
Sources
- MedlinePlus. Bunions. U.S. National Library of Medicine. https://medlineplus.gov/bunions.html
- American Orthopaedic Foot & Ankle Society (AOFAS). Hallux Valgus. https://www.aofas.org
- Cochrane Library. Interventions for treating hallux valgus. https://www.cochranelibrary.com
- American Podiatric Medical Association (APMA). Choosing the right shoes. https://www.apma.org
- National Center for Biotechnology Information (NCBI). Osteoarthritis of the first MTP joint / Hallux rigidus and related reviews. https://www.ncbi.nlm.nih.gov
- Peer-reviewed clinical reviews on hallux valgus recurrence and orthotic management (see NCBI and professional society guidance). https://www.ncbi.nlm.nih.gov
Want to share your experience?
Have you had a recurring bunion or been told you’re losing cartilage in the big toe? What helped — sleeves, orthotics, or surgery? Share your experience to help others choose practical next steps.
```